
This guide explains when they should consider testing, what a specialist adds, and how to choose the right next step.
What is sleep apnea, and why does it matter?
Sleep apnea is a condition where breathing repeatedly stops or becomes shallow during sleep, and a sleep apnea test Canberra can help identify whether these interruptions are occurring. It matters because these episodes reduce oxygen, fragment sleep, and strain the heart and brain over time.
Untreated sleep apnea is linked with high blood pressure, cardiovascular risk, daytime fatigue, and poor concentration. For some people, it also increases the risk of driving or workplace accidents due to microsleeps.
What symptoms suggest they might need a sleep apnea test in Canberra?
They should consider testing if they have loud snoring plus daytime symptoms, or if a partner has noticed breathing pauses. The key clue is unrefreshing sleep even after a full night in bed.
Common signs include morning headaches, dry mouth, frequent nighttime urination, irritability, poor focus, and excessive sleepiness. Some people mainly notice anxiety-like symptoms, low mood, or a constant “wired but tired” feeling.
When should they see a specialist rather than just “wait and see”?
They should see a specialist when symptoms are persistent, worsening, or affecting safety, work, or relationships. A specialist is also important when there are medical risk factors or complex sleep issues that need tailored care.
It is especially worth seeing a specialist if they have high blood pressure, atrial fibrillation, type 2 diabetes, significant obesity, or loud snoring with witnessed apneas. If they have ever nodded off while driving, that is an urgent sign to act.
Who is at higher risk of sleep apnea?
Risk increases when the airway is more likely to narrow during sleep. Anatomy, weight, hormones, alcohol, and certain medications can all contribute.
Higher-risk groups include people who snore loudly, those with a larger neck circumference, post-menopausal women, and anyone with nasal obstruction or jaw structure that reduces airway space. Family history also matters, and so does sleeping on the back.
What types of sleep apnea tests are available in Canberra?
Most people start with either a home sleep apnea test or an in-lab sleep study. The right option depends on symptoms, medical history, and how complex the case appears.
Home tests are convenient and often suitable when obstructive sleep apnea is strongly suspected. In-lab studies measure more signals and are usually preferred when they have other sleep disorders, significant lung or heart disease, neurological concerns, or when earlier results were unclear.
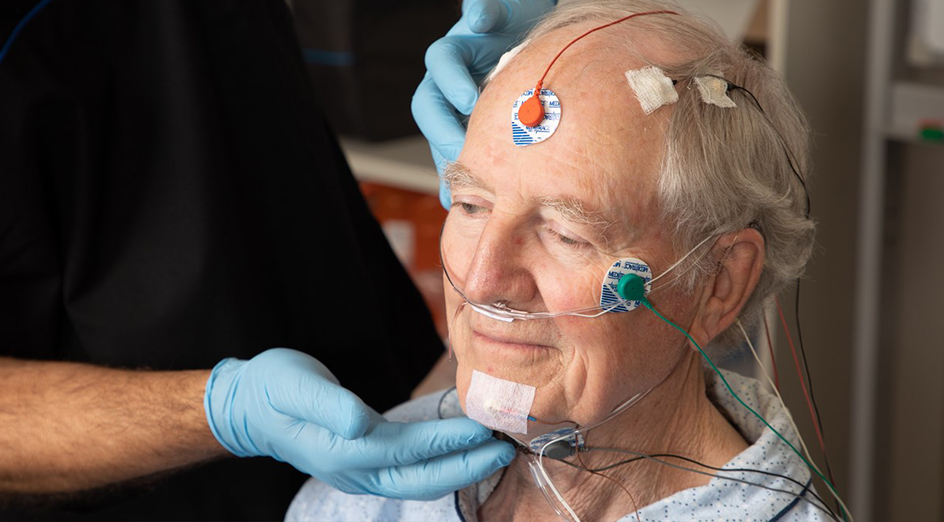
What happens during a home sleep apnea test?
A home test typically involves wearing sensors overnight to track breathing, oxygen levels, and heart rate. It is designed to capture whether breathing is repeatedly reduced or stopped.
They usually pick up the device or have it delivered, follow set-up instructions, then return it for scoring. If the data quality is poor, they may need to repeat it, which is one reason a specialist-led pathway can reduce delays.
What does a specialist do that a basic test cannot?
A specialist looks beyond a single number and matches results to symptoms, risks, and treatment preferences. They also rule out other causes of fatigue and can identify overlapping sleep problems.
They can interpret borderline studies, decide when an in-lab study is needed, and guide options such as CPAP, oral appliances, positional therapy, weight strategies, and nasal or ENT review. They also help with follow-up to make sure treatment is actually working.
How do they know it is time to book testing now?
They should book now if symptoms are affecting daytime function or if someone has noticed choking, gasping, or breathing pauses at night. Waiting often means months of avoidable fatigue and ongoing health strain.
A practical trigger is this: if they snore loudly and feel tired most days, testing is reasonable. If they have cardiovascular risks, diabetes, or safety concerns like drowsy driving, it is a priority.
What results might they receive, and what do they mean?
Results often include an index that reflects how often breathing events occur each hour and how low oxygen drops. These results help classify severity and shape treatment decisions.
Even “mild” sleep apnea can be significant if symptoms are strong or oxygen drops are meaningful. A specialist will usually weigh symptoms and risk profile, not just severity labels, before recommending a plan.
What treatments might follow a confirmed diagnosis?
Treatment aims to keep the airway open and restore normal sleep quality. The most common and effective treatment for many people is CPAP therapy.
Other options may include a mandibular advancement device fitted by a qualified dentist, positional therapy if events happen mainly on the back, addressing nasal obstruction, and weight management where relevant. The best plan is the one they can tolerate consistently.
How should they choose between a GP referral and going straight to a sleep specialist?
A GP is a good first step for many people, especially if they need a referral, a Medicare pathway, or assessment of other health issues. Going straight to a specialist can be helpful when symptoms are severe, complicated, or time-sensitive.
If they are unsure, they can start with a GP and ask for a clear plan: which test is recommended, how results will be reviewed, and what happens next if the test is negative but symptoms remain.
What should they do before their appointment or test?
They should note symptoms, sleep habits, and any partner observations in advance. This makes it easier to choose the right test and avoid repeat studies.
They can also list medications, alcohol intake, nasal congestion issues, and typical sleep times. If possible, they should bring information about blood pressure readings, existing heart or metabolic conditions, and any history of insomnia or restless sleep.
When is follow-up just as important as the test itself?
Follow-up matters because diagnosis is only the beginning. Many people struggle with mask comfort, pressure settings, or consistency, and small adjustments can make the difference between quitting and succeeding.
They should expect a review of symptoms, device data if using CPAP, and ongoing checks for blood pressure and daytime sleepiness. If treatment does not improve how they feel, they should ask whether another sleep issue is present or whether therapy needs refinement.
FAQs (Frequently Asked Questions)
What is sleep apnea and why is it important to get tested in Canberra?
Sleep apnea is a condition where breathing repeatedly stops or becomes shallow during sleep, leading to reduced oxygen levels, fragmented sleep, and strain on the heart and brain. Testing in Canberra is crucial because untreated sleep apnea can cause high blood pressure, cardiovascular risks, daytime fatigue, poor concentration, and increased risk of accidents due to microsleeps.
What symptoms indicate that I should consider a sleep apnea test in Canberra?
You should consider testing if you experience loud snoring accompanied by daytime symptoms such as morning headaches, dry mouth, frequent nighttime urination, irritability, poor focus, excessive sleepiness, or if a partner has noticed breathing pauses during your sleep. Unrefreshing sleep despite a full night in bed is also a key sign.
When should I see a specialist for sleep apnea rather than just waiting?
See a specialist when symptoms are persistent, worsening, or impacting safety, work, or relationships. It’s especially important if you have medical risk factors like high blood pressure, atrial fibrillation, type 2 diabetes, significant obesity, loud snoring with witnessed apneas, or if you have nodded off while driving. Specialists provide tailored care for complex cases.
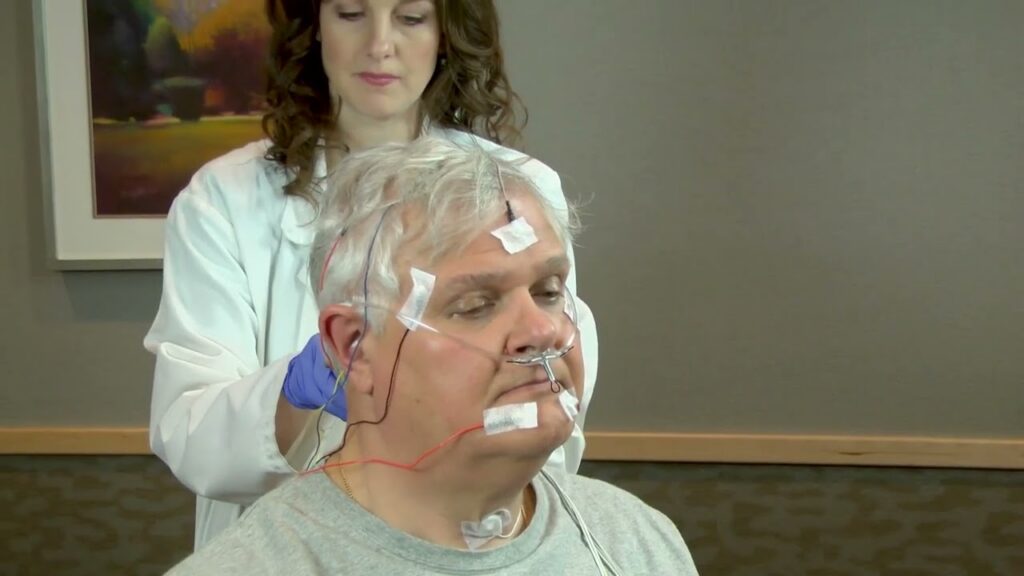
What types of sleep apnea tests are available in Canberra and how do I choose the right one?
In Canberra, you can start with either a home sleep apnea test or an in-lab sleep study. Home tests are convenient and suitable when obstructive sleep apnea is strongly suspected. In-lab studies are preferred for complex cases involving other sleep disorders or significant health issues. The choice depends on your symptoms, medical history, and case complexity.
What treatments are available after a confirmed diagnosis of sleep apnea?
Treatment aims to keep the airway open and restore normal sleep quality. The most common effective treatment is CPAP therapy. Other options include mandibular advancement devices fitted by qualified dentists, positional therapy if events occur mainly when sleeping on the back, addressing nasal obstruction, and weight management. The best treatment plan is one that you can tolerate consistently.
How do I prepare for my appointment or sleep apnea test in Canberra?
Before your appointment or test, note your symptoms, sleep habits, and any observations from your partner to help choose the right test and avoid repeat studies. List medications you’re taking, alcohol intake, nasal congestion issues, typical sleep times, blood pressure readings if available, existing heart or metabolic conditions, and any history of insomnia or restless sleep.
See Also: Sleep test Sydney: 5 warning signs you shouldn’t ignore.