ABSTRACT
Ten children between the ages of 8 and 19 with Lyme disease presented with chronic gastrointestinal symptoms. Biopsy evidence of inflammation was found in the stomach, duodenum, and colon. Pathologies included gastritis, duodenitis, gastric ulcer, colitis and histopathology resembling Crohn’s disease. Spirochetes with the microscopic appearance of Borrelia were found in five patients with chronic inflammatory conditions of the gastrointestinal tract. The inflammation may have been due to the spirochete itself, a reactive product related to their presence in the gastrointestinal tract or a consequence of medications used to treat Lyme disease.
INTRODUCTION
Lyme disease can affect a wide range of organ systems, producing dermatologic, musculoskeletal, neurologic, genitourinary, respiratory, cardiovascular and ocular manifestations (1). Reports of gastrointestinal (GI) manifestations have been limited to the liver and the spleen thus far. (2,3). To address the possibility of direct involvement of the GI tract, a retrospective study was made of children who had Lyme disease and chronic abdominal pain.
METHODS
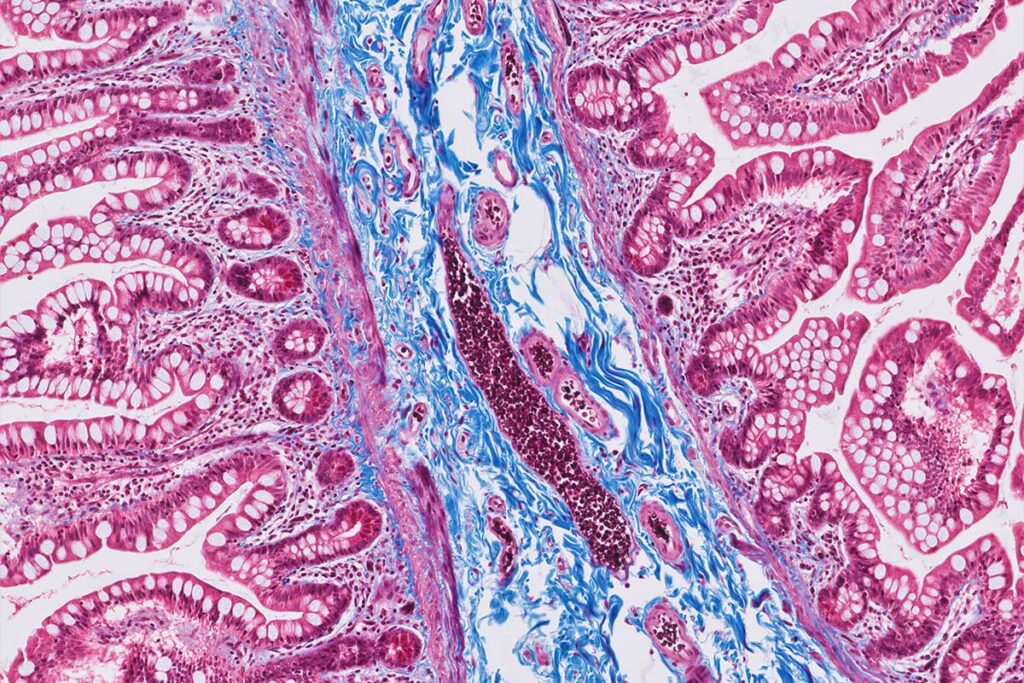
All patients included in our study had a physician documented erythema migrans rash and a positive western blot test (4) and were referred to the pediatric gastroenterology and nutrition service of Jersey Shore Medical Center for evaluation of chronic abdominal pain. The records of 400 children were examined and 10 patients satisfying the listed criteria were retrospectively identified ( 2 boys, 8 girls; mean age 15 +/- 4 years, range 8 to 19). Each case record included a history, physical examination, complete blood cell count, liver function tests, ultrasonography of the abdomen, upper gastrointestinal radiograph series with small bowel follow through, esophagogastroduodenoscopy (EGD) and colonoscopy. Stool samples were examined for occult blood, Salmonella, Shigella, Yersinia, Campylobacter, ova and parasites, and Clostridium difficile toxin. Gastrointestinal biopsies were reviewed to assess the GI mucosa by microscopy and whether Helicobacter pylori ( on EGD only) or spirochetes were present. Spirochetes were detected in tissue biopsy specimens using a modified Dieterle Stain (5).
Biopsy specimens were reported as acutely inflamed when polymorphonuclear cells were present in increased numbers and chronically inflamed if plasma cells and lymphocytes were present in increased numbers without an increase in polymorphonuclear cells. Depending on the depth of penertration of the inflammatory cells, severity of the inflammation was graded as mild ( superficial mucosa), moderate (lamina propria) or marked ( deeper than the lamina propria).
RESULTS
In all of the patients, abdominal pain began 1 month to 4 years before the diagnosis( median, 6 months before diagnosis) and before the initiation of antibiotics or non steroidal anti-inflammatory drugs (NSAIDs). Ultrasonography of the abdomen did not reveal any gallstones or pancreatitis. Serum bilirubin, alkaline phosphatase, alanine aminotransferase and aspartate aminotransferase and amylase levels were normal in all patients. Upper gastrointestinal series with small bowel follow through did not reveal a gastric or duodenal ulcer or terminal ileal disease. Endoscopy revealed evidence of inflammation in the stomach, duodenum, or colon in all of the patients. Click here to discover the health benefits of dairy delicacies.
Spirochetes consistent with the microscopic appearance of Borrelia burgdorferi were identified in the antrum of the stomach, the duodenum and the colon and were associated with chronic inflammation at these sites.
Two patients with chronic gastritis had H. pylori identified in the gastric antrum on biopsy. In one of these, H. pylori and spirochetes were present in both the stomach and intestines. The latter patient had been diagnosed with Lyme disease after the occurrence of an erythema migrans rash 2 years before and had completed a 1 month course of intravenous antibiotics prior to EGD.
In four patients who had chronic diarrhea and chronic abdominal pain, no laboratory evidence of , Salmonella, Shigella, Yersinia, Campylobacter, ova and parasites, and Clostridium difficile toxin was found in the stool. These patients had visibly evident blood on several occasions. In three patients, colonoscopy revealed mild to moderate chronic colitis. Spirochetes consistent with B. burgdorferi were present in the descending colon in one patient with colitis.
In the fourth patient with abdominal pain, Lyme disease, and chronic diarrhea, biopsies revealed areas throughout the entire colon with patchy active inflammation and cryptitis. Mutliple lymphoid aggregates were seen, however, no granulomas were identified. These findings were believed to resemble active Crohn’s disease ( at another institution) and were treated with daily oral prednisone for 4 weeks. The gastrointestinal symptoms improved, but the patient developed Bell’s palsy, chest pain, arthritis of the knee, heart palpitations, photophobia, tinnitus, stiff neck, an antalgic gait and foot drop. One year after this presentation, blood reappeared in the stool. Colonoscopy biopsies that were independently evaluated by pathologists at Jersey Shore Medical Center and at Brigham and Women’s Hospital revealed a chronic mucosal inflammation limited to the ascending colon, with no crypt abscesses, or evidence of granuloma formation or submucosal involvement.

DISCUSSION
Abdominal pain and the associated GI pathology in children with Lyme disease has not been reported previously. Spirochetes that are not Borrelia have been detected in the GI tract previously (6-8). Patients with gastric syphillus have presented with abdominal pain, vomiting and weight loss (7) and endoscopic findings range from minimal erythema to deep ulceration. In another report, colorectal spirochetosis was associated with chronic diarrhea without other intestinal symptoms (8).
We found strong histopathologic evidence that the Borrelia organisms were present in our biopsy samples. In 5 of 10 cases, we found spirochetes with the microscopic appearance of Borrelia and a characteristic morphology enabling differentiation from other spirochetes that could have been present. In addition, we found an increased number of plasma cells and lymphocytes in tissue biopsies, a pattern that is seen in other tissues infected by B. burgdorferi(9,10). B. burgdorferi could contribute to GI symptoms by its presence in the GI tract or by its ability to elicit a humoral, inflammatory or immune response anywhere along the entire GI tract (11). Duray and Steere (9) have proposed that B. burgdorferi can elicit interleukin-1, collagenase, prostaglandin E2, and circulating immune complexes. An intermittent and varying degree of immune complex formation may continue long after an infection is gone (12), raising the possibility of a spectrum of disease expression from mild chronic inflammation to what appears histologically to resemble Crohn’s disease in the colon.
One of our patients illustrates this possibility. Patient 1 was initially treated for Crohn’s disease, although no clinical or laboratory evidence supported this diagnosis. In this case, treatment of the Lyme disease with antibiotics improved the condition of the colon from one involving its entire length with cryptitis to be one described as superficial mucosal involvement restricted to the ascending colon and sigmoid colon. In cases like this one, we suggest that an inflammatory or immune reaction as a result of Lyme disease could injure the colon initially and even with elimination of the organism, the injury may persist as a Crohn’s like condition because of circulating immune complexes, which have been found in other tissues of patients with Lyme disease(12).
A diagnosis of Crohn’s disease in a patient with a history of exposure to B. burgdorferi needs to be weighted carefully. If the inflammation in the colon is in fact an immune reaction to the organism, the use of steroids might be contraindicated because immune suppression might exacerbate the Lyme disease as may have occurred with patient 1. Another treatment of Crohn’s disease, sulfasalazine, inhibits prostaglandin synthesis and might be a better choice of drug to ameliorate the inflammatory process of patients with Lyme disease in the colon without causing immune suppression.
We found the spirochetes to be associated with chronic inflammation in 5 of 10 cases. Other causes of inflammation must also be considered. Medications used to treat Lyme disease also may contribute to GI manifestations. Patient 5 was taking naproxen, an NSAID for 2 years prior to endoscopy. On endoscopy, a 5 cm x 5 cm gastric ulcer was found. NSAIDS have been reported to cause gastro duodenal injury in children with juvenile rheumatoid arthritis(13). In patients with Lyme disease, colitis and abdominal pain, the colitis may also have been related to intravenous use of cefotaxime. The Physicians’ Desk Reference (14) reports a 1.4% incidence of colitis in patients using cefotaxime. NSAIDs and other medications used to treat Lyme disease pose a significant risk of GI complications and suggest a need for careful differential diagnosis in patients with Lyme disease and chronic Gastrointestinal symptoms.
In summary, all children and adolescent with Lyme disease and chronic abdominal pain, had evidence of inflammation on biopsy in the stomach,, duodenum or colon. We found spirochetes in biopsy samples obtained throughout the GI tract that had a microscopic appearance consistent with B. burgdorferi. The inflammatory reaction we describe may have been caused by the spirochetes, by immune system products elicited in response to spirochete presence or by medications used to treat Lyme disease. A careful differential diagnosis is recommended in all patients with Lyme disease and chronic abdominal pain or bloody diarrhea.
REFERENCES
- Steere AC. Lyme disease. N Engl J Med. 1989; 321: 586-596.
- Goellner et al. Hepatitis due to recurrent Lyme disease. Ann Intern Med. 1988; 108: 707-708.
- Cimmino MA et al. Spirochetes in the spleen of a patient with chronic Lyme disease. Am J Clin Pathol. 1989;91: 95-97
- Centers for Disease Control and Prevention. Lyme disease. MMWR. 1990; 39:21.
- Duray PH, et al. Demonstration of the Lyme disease spirochete Borrelia burgdorferi by a modification of the Dieterle stain. Lab Med. 1985; 16: 685.
- Ruane PJ et al. Spirochete like organisms in the human gastrointestinal tract. Rev Infect Dis. 1989;11:184-196.
- Winters HA et al. Gastric Syphillus: five recent cases and a review of the literature. Ann Intern Med. 1992; 116:314-319
- Dauzan YR, et al Colorectal spirochetosis is it an anatomopathologic entity? Ann Pathol. 1990;10:258-261.
- Duray PH, Steere AC. Clinical pathologic correlations of Lyme disease by stage. Ann NY Acad Sci. 1988;539: 65-79
- Van der Linde MR et al. Range of atrioventricular conduction disturbances in Lyme borreliosis. British Heart Journal. 1990; 63: 162-168.
- Defosse DL, Duray PH, Johnson RC. The NIH 3 immunodeficient mouse is a model for Lyme borreliosis myositis andcarditis. Am J Pathol. 1992; 141:3-10
- Johnson YE, Duray PH, Steere AC et al. Spirochetes found in synovial microangiopathic lesions. Am J Pathol. 1985; 118: 26-34.
- Mulberg Ak et al. Identification of non steroidal drug induced gastroduodenal injury in children with juvenile rheumatoid arthritis. J Pediatr. 1993; 122: 647-649.
- Barnhart E (ed). Physician’s Desk Reference, 47th Ed. Montvale, NJ. Medical Economics Company, INC 1991;1060.
More to read: Exploring the Benefits of CPAP Masks